Food Assistance: How Strong Is the Safety Net?
- by Michael LeBlanc, Biing-Hwan Lin and David Smallwood
- 9/1/2006
Highlights
- Food assistance programs, particu-larly the Food Stamp Program, increase food spending and household income.
- In 2004, adding food stamp benefits to recipients' incomes raised 9 percent of recipients out of poverty.
- Nutritional effects of food assistance programs are uncertain.
Born during the Great Depression, but growing to maturity during the 1960s, 1970s, and 1980s, food assistance programs have provided a safety net to help U.S. households purchase sufficient food. Safety nets are created for moral, economic, and political reasons. For economists, a safety net is a policy that ensures a minimum income, consumption, or wage level. Safety nets can be viewed as social insurance to help people through livelihood shocks and stresses, such as those caused by illness, unemployment, or job displacement.
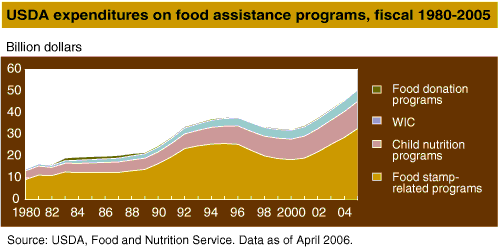
An original intent of food assistance programs was to increase food access and reduce food insecurity. During the last few decades, food assistance programs, particularly the school meals programs and the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC), have also been promoted as a nutrition safety net offering access to essential nutrients and minerals. In fiscal year 2005, Federal funding for the food assistance and nutrition programs was nearly $51 billion, comprising 55 percent of USDA’s budget. Farmers, food companies, and program participants have benefited from the increased food spending and improved food security. Evidence of improved nutrition for program participants is more difficult to demonstrate.
Food Assistance Increases Food Expenditures . . .
U.S. agriculture and nutrition policy includes a variety of farm programs and food assistance and nutrition programs that support an abundant food supply and affordable prices. The core food assistance programs, managed and funded by USDA, include the Food Stamp Program, the school meals programs, WIC, and commodity distribution programs. These programs serve one in every five Americans at some point during the year. The Federal Government partners with State and local, public, and private agencies to administer (and, in some cases, contribute funding for) its food assistance efforts. Each program has its own objectives, eligibility criteria, benefit structure, and legislative oversight.
The Food Stamp Program is the foundation of the food assistance safety net. It provides benefits to qualifying families and supports markets for agricultural products. With program costs of $31 billion in fiscal 2005, it is the country’s largest food assistance program. Using normal retail marketing channels, the Food Stamp Program provides qualified low-income households with increased purchasing power to acquire food. It offers the only form of assistance available nationwide to most households on the basis of financial need only, irrespective of family type, age, or disability. For many low-income households, the program is an important source of purchasing power. For a typical low-income family with children, food stamps provide about 25 percent of the family’s total purchasing power.
The Food Stamp Program increases household food expenditures. Not only does the program increase food expenditures beyond what households would spend without the program, households spend more on food than they would if the same amount of benefit were given as cash. A dollar of food stamp benefit is estimated to increase food spending by 17 to 47 cents, versus 5 to 10 cents from a dollar of cash assistance. Although the food stamps themselves must be spent on food, a dollar of food stamps does not lead to a dollar in additional food spending because cash previously spent on food can be used for rent, clothing, and other nonfood expenses.
. . . Reduces Food Insecurity . . .
Do food assistance programs reduce the probability that vulnerable households experience food insecurity? That is, do the programs lessen the likelihood that poor families have insufficient food for an active, healthy life for all household members? This question was recently answered by George Borjas of Harvard University through ERS-supported research. Borjas took advantage of a “natural experiment” when Federal welfare reform legislation limited the eligibility of immigrant households to receive assistance, while some States chose to continue offering State-funded assistance to immigrant households. Borjas exploited these changes in eligibility rules to examine the link between food insecurity and public assistance.
His research indicates that a 10-percentage-point cut in the share of the population that receives public assistance increases the share of food-insecure households by about 5 percentage points. Borjas’s research supports the hypothesis that food assistance programs are an important determinant of providing households with a minimal level of food sufficiency.
. . . and Raises Incomes
Food assistance programs reduce overall economic vulnerability, not just food insecurity—particularly during downturns in the business cycle. Individuals with longer term needs resulting from chronic illness, disability, or old age also rely on these assistance programs. Food assistance programs targeting those who may be temporarily affected when events take an unfavorable turn can be viewed as income insurance to help people through temporary livelihood shocks, such as those caused by illness or unemployment.
The Food Stamp Program is particularly helpful during economic downturns for households with stronger ties to the workforce. The amount of food stamps given to a household depends on the number of eligible people in a household and the household’s net income. A 4-person household with zero net income would receive the maximum food stamp benefit of $506 per month. If the family’s net income rose by $100 per month, its benefits would fall to $476.
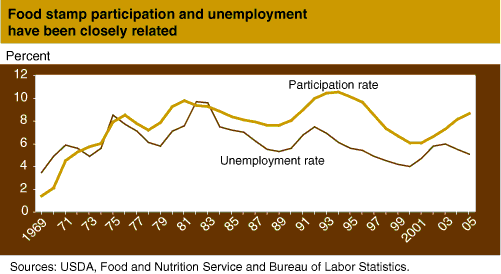
During a recession, as wages stagnate, work hours decrease, and jobs are lost, food stamp benefits increase for current participants, and more households become eligible. But how many people turn to the Food Stamp Program in the event of a recession? ERS research suggests the 1-year effect of a rise in unemployment by 1 percentage point is about 700,000 additional food stamp recipients. Over 5 years, the 1-percentage-point increase in unemployment leads to a total of 1.3 million additional recipients
A number of other studies indicate food assistance programs, particularly the Food Stamp Program, have significant positive effects on household income. Although recent evidence suggests a changing relationship between unemployment and food stamps, historically, program effects have been countercyclical. That is, more assistance is provided to households during a downturn in the economy and less during an economic expansion. A report by the Congressional Budget Office indicates that of all the federally funded assistance programs, for which participant eligibility depends on income and assets, only the Food Stamp Program was responsive to changing economic conditions.
Food stamps succeed in raising participants’ incomes. Adding the dollar value of food stamp benefits to the income of food stamp recipients yields a significantly different poverty distribution. In 2004, adding food stamp benefits to income was sufficient to raise 9 percent of food stamp recipients out of poverty. Food stamp benefits have an even greater impact on the poorest households, raising 17 percent of food stamp households above 50 percent of the poverty guideline.
Food Stamps Reduce Child Poverty
In 2000, 8.8 million U.S. children received food stamps. To illustrate the efficacy of food stamps in helping households meet basic needs, ERS researchers added the value of food stamp benefits to household income and then measured the effect on child poverty rates. This “food stamp effect” reduced the number of children in poverty in 2000 by 4 percent, lifting about 500,000 children out of poverty. Augmenting income with the value of food stamp benefits also has the effect of reducing the depth of child poverty by 20 percent or more, as measured by the reduction in the poverty gap or the amount of income needed to raise income to the poverty threshold.
Nutrition Studies Are Dated, Recent Results Are Mixed
The positive impacts of food assistance programs on food expenditures and incomes are clear. Less certain are the programs’ impacts on nutrition. ERS has released a series of reports providing the first systematic and comprehensive review of the hundreds of studies on the effects of various food assistance programs—especially the main four—on nutrition and health.
The WIC program provides low-income pregnant, breastfeeding, and postpartum women, infants, and children up to age 5 with specific supplemental foods, nutrition education, and referrals to health care and social services. Most studies indicate the WIC program—with its emphasis on iron-fortified infant formula, infant cereals, and ready-to-eat cereals—has helped reduce anemia in children. Further evidence suggests that WIC has improved children’s intakes of iron, vitamin B6, and folate, and reduced their intake of added sugar and fat. Recent studies, however, have failed to reproduce earlier work showing that women in WIC increased their intakes of food energy (calories), protein, vitamin C, iron, and calcium. Moreover, recent studies conducted using dietary assessment methods recommended by the Institute of Medicine indicate that, today, the vast majority of both WIC and non-WIC children have nutritionally adequate diets.
Schools that participate in the National School Lunch Program (NSLP) and School Breakfast Program receive cash and commodities from USDA to offset the cost of providing the meals. In return, the schools serve meals that meet Federal nutritional standards and offer free or reduced-price meals to low-income children.
Analyses of the impacts of the NSLP are anchored by two national evaluations: the National Evaluation of School Nutrition Programs, conducted in 1980-81, and the first School Nutrition Dietary Assessment Study, conducted in 1991-92. In addition to these national evaluations, studies have used national survey data or local data sets to assess impacts.
These evaluations strongly indicate that the NSLP increases children’s lunchtime intakes of riboflavin, vitamin B12, calcium, phosphorus, magnesium, and zinc. Evidence for riboflavin, calcium, and phosphorus is particularly strong. Every study that examined intakes of these nutrients found that NSLP participants had significantly higher intakes at lunch than non-participants. It is generally accepted that this pattern is caused by increased consumption of milk, which is a concentrated source of all of these nutrients and a feature of NSLP lunches, by participants.

However, NSLP operations changed substantially after most of the research on health benefits was completed. Responding to findings in the early 1990s that school lunches were high in fat, saturated fat, and sodium, and low in carbohydrates, USDA launched the School Meals Initiative for Healthy Children in 1995 to bring school lunches and breakfasts in line with the Dietary Guidelines for Americans. One cannot assume that findings from earlier research apply to today’s NSLP. An updated survey (currently underway by USDA) and new research are essential to understanding the impact of the NSLP as it operates today.
Studies prior to the School Meals Initiative indicate that the School Breakfast Program had no impact on the likelihood of a child’s eating breakfast, but availability of the program was associated with a greater likelihood that low-income students would eat a more substantial breakfast. The program was found to increase intakes of three minerals—calcium, phosphorus, and magnesium—both at breakfast and over 24 hours. (Riboflavin intake also increased at breakfast, but the effect did not persist over the full day.) All of these nutrients occur in concentrated amounts in milk.
The positive effect of the Food Stamp Program on food expenditures has been extensively analyzed and confirmed in many studies, with much of the research using large national surveys. But increased food spending does not necessarily lead to improved nutrition. The effect of increased food expenditures on household availability of food energy and nutrients is mixed. Early studies of the program found an effect on certain vitamins and minerals, while more recent studies of the program as it is currently structured show increases in the household availability of food energy and protein. Earlier studies indicate that the program may increase children’s intakes of vitamins and minerals, but these findings were not replicated in the most recent studies.
The most thorough studies of food assistance programs suggest mixed nutrition effects. Caution must be used in interpreting results, positive or negative, from most nutritional studies of food assistance programs. One cannot logically infer that food assistance programs have no nutritional effects from studies that fail to demonstrate positive effects.
Weak evaluation designs and/or inadequate data limit conclusions that can be drawn about causality between food assistance participation and nutrition and health outcomes (see “Prior Nutrition Research Has Limitations”). This is particularly true of longer term outcomes, such as iron deficiency (anemia) and weight status. Food assistance participation must precede such outcomes by long enough and be robust enough to provide a plausible impact. Reliable assessment of impacts requires measurements both before and after participation, preferably multiple measurements. In addition, nutrition outcomes are influenced by a complex interplay of economic, diet, genetic, and environmental factors, making it challenging to isolate the specific impact of food assistance programs.
This article is drawn from:
- Fox, M.K., Hamilton, W. & Lin, B. (2004). Effects of Food Assistance and Nutrition Programs on Nutrition and Health: Volume 4, Executive Summary of the Literature Review. U.S. Department of Agriculture, Economic Research Service. FANRR-19-4.
- Food Stamp Benefits and Childhood Poverty in the 1990s. (2003). USDA, Economic Research Service. FANRR-33. .
You may also like:
- Ver Ploeg, M., Mancino, L. & Lin, B. (2006, February 1). Food Stamps and Obesity: Ironic Twist or Complex Puzzle?. Amber Waves, U.S. Department of Agriculture, Economic Research Service.
- Hanson, K. & Gundersen, C. (2002). Issues in Food Assistance-How Unemployment Affects the Food Stamp Program. U.S. Department of Agriculture, Economic Research Service. FANRR-26-7.
- Ralston, K. (2006). Nutrient Adequacy of Children Participating in WIC. U.S. Department of Agriculture, Economic Research Service. EB-8.